Abcarian: I dodged COVID-19 for more than two years. The latest surge finally got me.

It was bound to happen.
The day after her Los Angeles middle school let out for the summer, my irrepressible 12-year-old niece, who lives with me, was feverish and lethargic. This was so unfair.
For more than two years, she’d been an absolute beast about wearing her mask, declining to pull it down for photos, forgetting to take it off at home, perplexed by the mask refuseniks.
Just three days earlier, she’d tested negative for COVID-19 at school. Then, suddenly, positive.
Her symptoms were mild, and frankly, she wasn’t too upset at first because she equates being sick with watching television, drinking ginger ale and eating ice cream.
However, once she realized she would not be able to join family for a long-planned trip to Disneyland, she basically lost it. I kept my distance from her and did not change my weekend plans, which was probably a mistake.
That evening, I co-hosted a college graduation party for my step-granddaughter. The next, I had dinner with my daughter and former stepmother. (We steered clear of my niece; the party took place in a friend’s backyard, and the dinner was served in the little mother-in-law apartment above my garage.)
On Tuesday morning, I woke up with a sore throat, slight fever and the sinking feeling that my luck had run out. Two red lines on the rapid antigen test confirmed it.
With two vaccines and one booster shot under my belt, how sick would I get?
And what should I do?
::
Chances are you know someone who has COVID-19 right now.
California’s current surge, reports my colleague Luke Money, is the third-highest peak of the entire pandemic. Blessedly, fewer people are becoming seriously ill, getting hospitalized or dying.
That’s because we now have vaccines, readily available home tests and, of course, antiviral medications for those at risk of becoming seriously ill.
In the spring, the state of California, Los Angeles County and the city of L.A. all stopped requiring proof of vaccination to enter public spaces like restaurants and gyms (the exception is large indoor events with more than 1,000 people). Mask mandates were dropped, although public health officials never stopped recommending them for indoor public places.
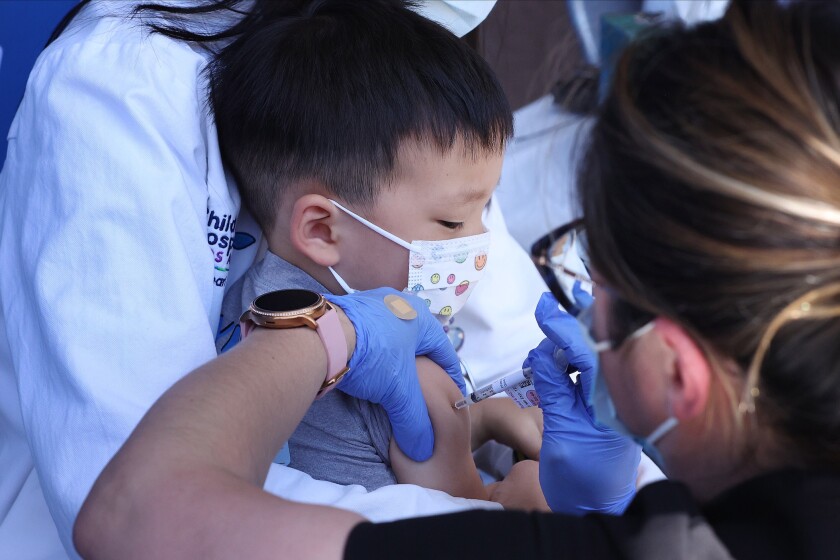
The final major phase of the COVID-19 vaccination campaign kicked off this week, with California finally able to inoculate children under 5.
After many months of pandemic anxiety and precautions, I let my guard down. I forgot to wash my hands. I stopped wearing a mask and, frankly, stopped worrying about contracting an infection. I’d read that immunologists theorize that some portion of the population might not be susceptible to COVID-19, and I lulled myself into thinking I might be one of those with “super-immunity.”
And yes, I laughed when I wrote that just now.
::
By the second day, my symptoms were worsening, and I was kicking myself for not getting that second booster. I decided to see if I could get a prescription for Paxlovid, the new antiviral that friends told me I needed.
I don’t have a regular internist right now, so I decided to find a nearby “Test to Treat” center. The federally funded sites are scattered around — in pharmacies and clinics — but I wasn’t up to driving anywhere. Also, the first pharmacy I called put me on hold for 15 minutes before disconnecting.
I decided to call the county health department at (833) 540-0473. My call was answered on the second ring. I was assigned a case number and transferred to a nurse, who took my medical history.
About 20 minutes later, a physician, Dr. Hang Tran, called me back and discussed my symptoms, current medications and offered to call in a prescription for Molnupiravir, one of two antivirals effective in combating COVID-19. Paxlovid, she said, was contraindicated for me because of the statin drug I take.
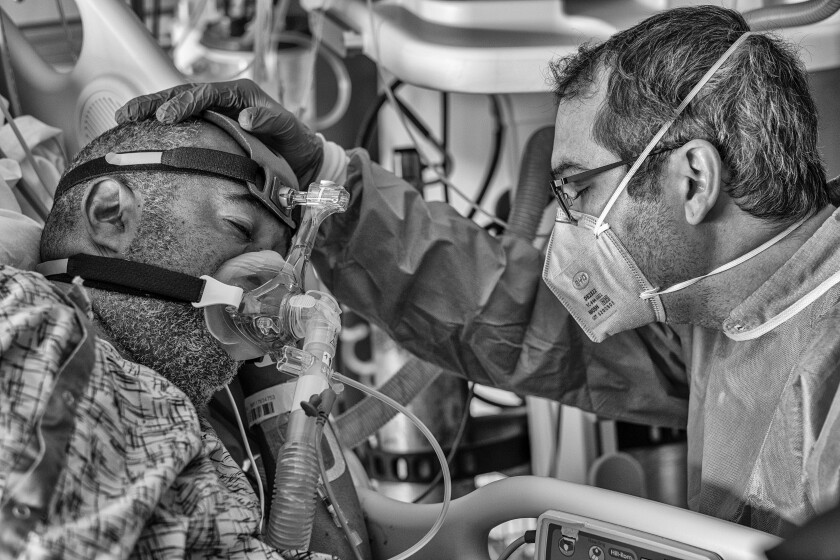
Despite the latest surge in coronavirus cases, the impact on hospitals has been relatively minor and COVID-19 deaths have remained fairly low and stable.
Both medicines have been issued emergency-use authorizations by the Food and Drug Administration to treat people with mild to moderate COVID symptoms who are at high risk of developing more severe symptoms, which includes anyone 65 and older and people with a wide variety of underlying conditions. The drugs must be started within five days of the onset of symptoms, preferably as soon as symptoms appear.
A little over an hour after Dr. Tran and I hung up, my friend Dayle tossed a bag onto my kitchen counter. “Here you go!” she sang as she scurried away.
The following day, a public health nurse called to check up on me. I was astonished. I have had outpatient surgeries where no one bothered checking in like that.
“I’m glad you had such a positive experience, that’s exactly what we are trying to create,” said Dr. Seira Kurian, a regional health officer for the county Department of Public Health. The county’s COVID telehealth program, she told me, is only a couple months old. “Because therapeutics require a prescription, we realized early that this would be an issue for individuals like yourself, or who have no access to healthcare, or are underinsured or uninsured.”
How to process the pandemic death toll? For one hospital chaplain, it means also remembering relatives left behind.
If a sick person has no one to pick up the meds, Kurian said, there’s a solution — the county has partnered with FedEx to deliver supplies overnight.
Callers were scarce in the beginning, she said, but infection rates have surged and word is getting around. As of last week, she said, the program has served about 1,000 patients. I count myself lucky to be among them.
The couple with whom I co-hosted the graduation party tested positive, are moderately ill and are isolating with antivirals.
The 12-year-old isolated for five days, tested negative and is happily ensconced in day camp.
I, on the other hand, am still a bit under the weather. My sore throat is gone, but seven days in, I’m still testing positive, which means I have to isolate for another three days. After that, even if I’m positive, the doctors tell me, I can leave the house.
And when I do, you can bet I will be wearing a mask.