Scientist uncovered nearly 200 genetic mutations of Coronavirus. But, what does it mean?
The study, published in journal Infection, Genetics and Evolution, characterized patterns of diversity of the genome of the virus, highlighting how it may be adapting and evolving to its human hosts
In a combined study, scientists have identified 198 mutations that appear to have independently occurred more than once, which may hold clues to how the SARS-CoV-2 is adapting. The study was based on the analysis of the virus genes from over 7,500 people infected with the disease globally. This kind of study is not uncommon as it offers clues to direct drugs and vaccine targets, but it is commonly done in a much wider time-frame.
The study, led by the University College London, the UCL Genetics Institute, and published in the journal Infection, Genetics and Evolution, characterized patterns of diversity of the genome of the virus, highlighting how it may be adapting and evolving to its human hosts.
Co-lead author Professor Francois Balloux (also from UCL Genetics Institute) said: “All viruses naturally mutate. Mutations in themselves are not a bad thing and there is nothing to suggest SARS-CoV-2 is mutating faster or slower than expected. So far we cannot say whether SARS-CoV-2 is becoming more or less lethal and contagious.“
The researchers found that a large proportion of the global genetic diversity of SARS-CoV-2 is found in all hardest-hit countries, suggesting extensive global transmission from early on in the epidemic and the absence of single ‘Patient Zeroes‘ in most countries.
The findings further establish that the virus only emerged recently in late 2019, before quickly spreading across the globe.
Should the Coronavirus mutations be concerning?
The quick answer is no. The small genetic changes, or mutations, identified were not evenly distributed across the virus genome, the researchers said.
As some parts of the genome had very few mutations, those invariant parts of the virus could be better targets for drug and vaccine development,
“A major challenge to defeating viruses is that a vaccine or drug might no longer be effective if the virus has mutated. If we focus our efforts on parts of the virus that are less likely to mutate, we have a better chance of developing drugs that will be effective in the long run,” Balloux explained. “We need to develop drugs and vaccines that cannot be easily evaded by the virus,” he said.
“There are still very few genetic differences or mutations between viruses,” co-lead author Lucy van Dorp from UCL added. “We found that some of these differences have occurred multiple times, independently of one another during the course of the pandemic — we need to continue to monitor these as more genomes become available and conduct research to understand exactly what they do,” said Dorp.
The results add to a growing body of evidence that SARS-CoV-2 viruses share a common ancestor from late 2019, suggesting that this was when the virus jumped from a previous animal host into people.
This means it is most unlikely the virus causing Covid-19 was in human circulation for long before it was first detected, the researchers said.
As per today, there are three lineages of Coronavirus identified as a result of its mutations
Scientists have reconstructed the early “evolutionary paths” of COVID-19 as the infection spread from Wuhan, out to Europe and North America, an advance that sheds light on the mutations undergone by the novel Coronavirus since its origin.
According to the researchers, including those from the University of Cambridge in the UK, there are three distinct “variants” of COVID-19, consisting of clusters of closely related lineages, which they labeled ‘A’, ‘B’ and ‘C’.
By analyzing the first 160 complete virus genomes to be sequenced from human patients, the study, published in the journal PNAS, mapped some of the original spread of the new SARS-CoV-2 through its mutations into the lineages.
“There are too many rapid mutations to neatly trace a COVID-19 family tree. We used a mathematical network algorithm to visualize all the plausible trees simultaneously,” said geneticist Peter Forster, lead author of the study from the University of Cambridge.
“These techniques are mostly known for mapping the movements of prehistoric human populations through DNA. We think this is the first time they have been used to trace the infection routes of a virus,” Forster said.
The scientists used data from virus genomes sampled from across the world between 24 December 2019 and 4 March 2020.
According to Forster and his team, the closest type of COVID-19 to the one discovered in bats — type ‘A’, the “original human virus genome” — was present in Wuhan, but surprisingly was not the city’s predominant virus type.
They said mutated versions of ‘A’ were seen in Americans reported to have lived in Wuhan, and a large number of A-type viruses were found in patients from the US and Australia.
Wuhan’s major virus type, ‘B’, was prevalent in patients from across East Asia but the variant didn’t travel much beyond the region without further mutations.
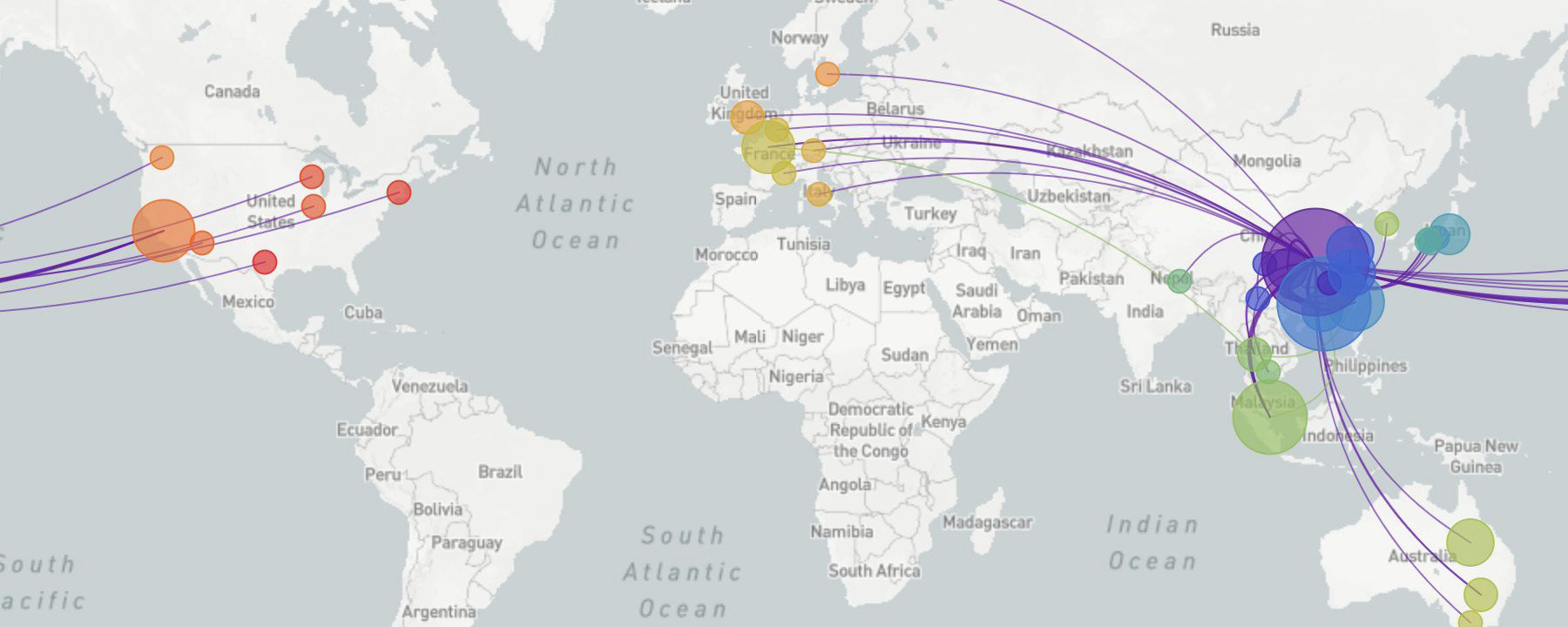
Based on this, the scientists said there could have been a “founder event” in Wuhan, or “resistance” against this type of COVID-19 outside East Asia.
The ‘C’ variant, they said, is the major European type, found in early patients from France, Italy, Sweden, and England. It is absent from the study’s Chinese mainland sample but seen in Singapore, Hong Kong, and South Korea.
The study also suggested that one of the earliest introductions of the virus into Italy came via the first documented German infection on January 27 and that another early Italian infection route was related to a “Singapore cluster”.
One particular strain is worrying experts
Preliminary research from Los Alamos National Laboratory in US’s New Mexico, focusing on genetic changes or mutations in the “Spike” protein that gives the virus its distinctive “crown-like” shape, has identified 14 mutations in the Spike. The research was done using a database called the Global Initiative on Sharing All Influenza Data (GISAID). According to the researchers, one particular mutation — identified as D614G — is of “urgent concern“. “It began spreading in Europe in early February, and when introduced to new regions it rapidly becomes the dominant form,” according to the study, which has not yet been peer-reviewed.
 There are reports that an analysis of 82 strains of the virus in India by India-born Prof. S.S. Vasan and his colleagues from the Commonwealth Scientific and Industrial Research Organisation (CSIRO) in Australia showed that nearly 50 percent of them have the new mutation, while globally, nearly two-thirds of all strains have displayed this mutation.
There are reports that an analysis of 82 strains of the virus in India by India-born Prof. S.S. Vasan and his colleagues from the Commonwealth Scientific and Industrial Research Organisation (CSIRO) in Australia showed that nearly 50 percent of them have the new mutation, while globally, nearly two-thirds of all strains have displayed this mutation.
The researchers have proposed increased transmissibility of the virus due to the mutation. “D614G is increasing in frequency at an alarming rate, indicating a fitness advantage relative to the original Wuhan strain that enables more rapid spread,” according to the study. This essentially means that viruses bearing the mutation D614G are replacing the original Wuhan form of the virus rapidly and repeatedly across the globe. “Based on currently available information, there are several ways the D614G mutation may impact Spike’s infectivity: it may improve receptor binding, fusion activation, or ADE antibody elicitation.”
Will it affect vaccine development?
Experts have suggested it should not. Mutations, to an extent, do not affect vaccine development. Take seasonal influenza. Because of mutations, vaccines have to be tweaked every year to target it against the then-dominant strain. Also, as mentioned before, scientists could target the unmutated or invariant parts of the virus for better vaccine development.
The Head of Epidemiology and Communicable Diseases at ICMR, Dr. Raman R. Gangakhedkar had earlier said, “It will take some time for us to know the predominant quasi-species of the novel Coronavirus in the world. But mutations are not likely to make potential vaccines ineffective, as all sub-types of the virus have the same enzymes.“

A theory debunked?
On a different front, a study by scientists at Britain’s Glasgow University, analyzing mutations in the SARS-CoV-2 genomes, claimed that the mutations found did not signal that there were completely different strains of the virus. This was a direct push back against a previous Chinese study, which claimed there were two separate strains of the virus, one more infectious and virulent than the other.
The difference between a virus strain and a virus variant is it the serotypes of the same virus (e.g., various antibody neutralization phenotypes). The variant is a virus whose phenotype differs from the original wild-type strain but the genetic basis for the difference is not known, for example, a new clinical isolate from a patient.
The almost 200 mutations do not necessarily change the virus enough to be defined as a new strain. However, the evolutionary path of the virus can result in different variant types (labeled above as types ‘A’, ‘B’, and ‘C’), which is important to track to maintain focus on the similarities as it affects how vaccines are produced. The proposed virus strain (below labeled as ‘L’ and ‘S’) are more troublesome differences because it may change the virus behavior and inevitability, and may also affect vaccines as one strain can be resistant to a vaccine created to protect against another strain.
The study, ‘On the origin and continuing evolution of SARS-CoV-2’, published in National Science Review, had hypothesized that there were two strains of the virus — ‘L’ and ‘S’. According to the study, the aggressive L type of Coronavirus was found more in the early stages of Wuhan outbreak, but its frequency decreased due to human intervention. “Whereas the L type was more prevalent in the early stages of the outbreak in Wuhan, human intervention may have placed more severe selective pressure on the L type, which might be more aggressive and spread more quickly. On the other hand, the S type, which is evolutionarily older and less aggressive, might have increased in relative frequency due to relatively weaker selective pressure,” according to the study.
According to the Glasgow study: “A recent study by Tang et al. (2020) claimed that two major types of SARS-CoV-2 had evolved in the ongoing COVID-19 pandemic and that one of these types was more “aggressive” than the other. Using examples from other viral outbreaks, we discuss the difficulty in demonstrating the existence or nature of a functional effect of a viral mutation, and we advise against over-interpretation of genomic data during the pandemic.“
Experts in Gujarat had hypothesized that this more aggressive Wuhan L strain was one reason behind the higher COVID-19 mortality rates. “Analysis done by scientists abroad has shown that the L-type strain has been dominant where more mortality is reported among Coronavirus patients. This strain was found to be more prevalent in Wuhan,” director of state-run Gujarat Biotechnology Research Centre (GBRC) C.G. Joshi said.
Conclusion
We know quite a bit about the SARS-CoV-2 already, but yet not enough to determine the best way to create definitive vaccines, treatments, or more effective prevention methods. Everyone is doing the best they can, and those six months (which feels more like six years) has been incredible in terms of knowledge acquisition, despite tragic and scary.

But, here the ultimate truth: our last hope lies in science. It is not faith, not belief, nor it is desire or strength. By far it is not political orientation! Only science can ultimately save us all! We must maintain the energy and investment in all possible fronts, studying this virus through all extremes, keep thinking out of the box and exploring our technologies to the extreme, keep exchanging information, cooperating and supporting each other. Only by keeping doing what we are doing we will be able to gather enough proven data to create an efficient strategy to combat and kill this beast. Otherwise, mankind may stay as a hostage of its will for a very long time.


