Kawasaki Disease linked to COVID-19 in Kids
Pediatricians, immunologists, and cardiologists are keeping a close watch on pediatric cases that look similar to Kawasaki syndrome following reports that draw a tenuous link between the inflammatory arterial disease and COVID-19 in children.

As health organizations have started warning about unusual presentations of a Kawasaki disease-like inflammatory syndrome associated with COVID-19, some pediatric cardiologists noted that even classic cases are likely going undercounted.
What is Kawasaki disease?
Kawasaki disease is a rare pediatric inflammatory condition that results in swelling throughout the body’s arteries, including those that lead to the heart. It also affects the lymph nodes, skin, and mucous membranes, according to the Mayo Clinic.
Early symptoms typically include fever, skin rash, red eyes, cracked lips, and swelling; as the disease progresses, symptoms can also include peeling skin, gastrointestinal distress, and joint pain.
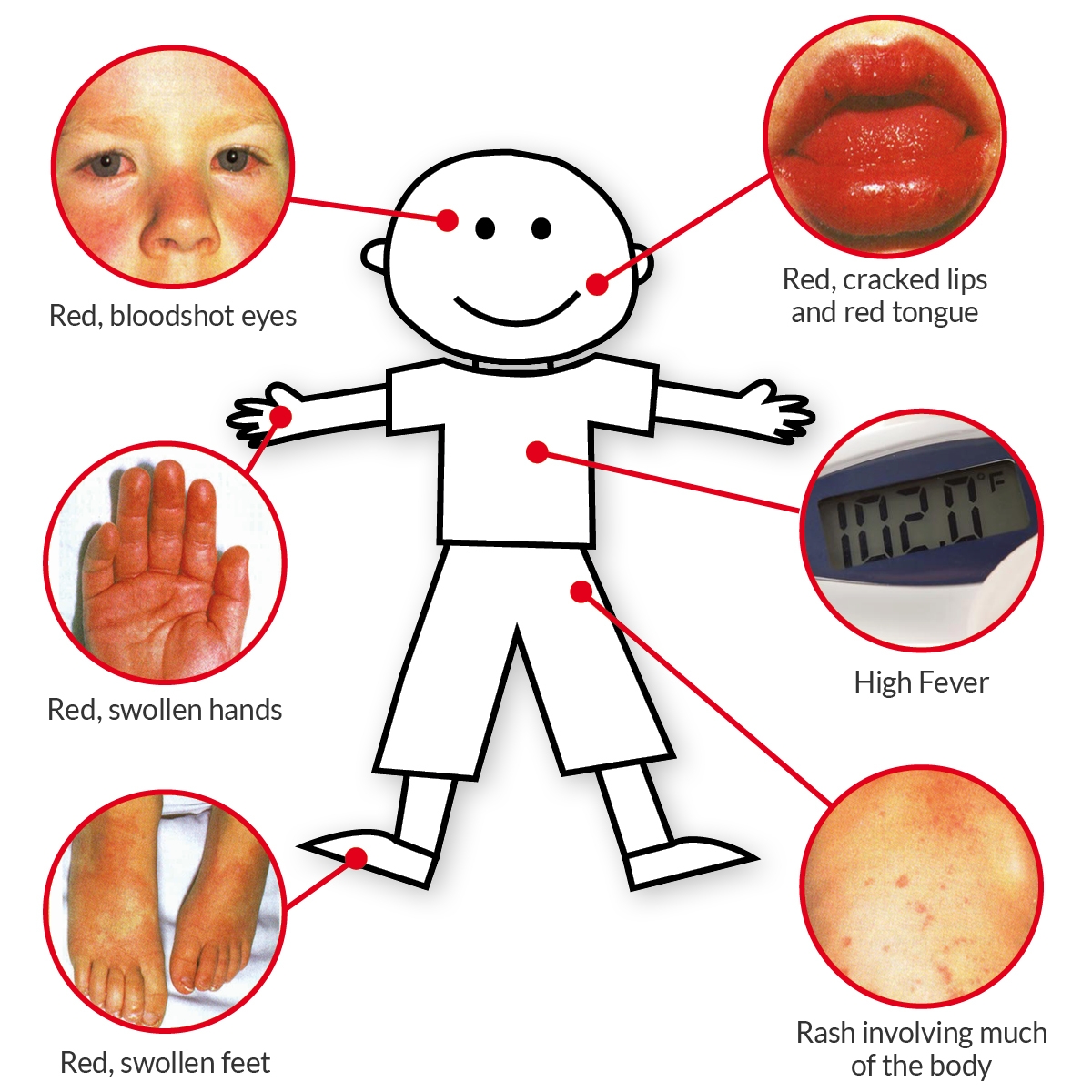
About 3,000 cases of Kawasaki disease are diagnosed each year in the U.S., according to the National Organization for Rare Disorders. It predominantly affects children ages five and younger, and is more common among boys than girls.
Dr. Veena Goel Jones, a pediatric hospitalist with Palo Alto Medical Foundation in California, explains that if left untreated Kawasaki can lead to serious cardiac complications. But with medical attention, it’s usually easily treated with anti-inflammatory drugs.
What’s the relationship between Kawasaki and COVID-19?
That’s still under investigation. But Dr. Roshni Mathew, Jones’ colleague and a pediatric infectious disease specialist at Stanford’s Lucile Packard Children’s Hospital, says “the general thought is this is a post-infectious trigger causing the immune system to hyper-react.” Infections of any kind can cause inflammation in the body. So it’s possible that SARS-CoV-2, the virus that causes COVID-19, is kickstarting Kawasaki-like inflammatory responses in small numbers of children, she says.
Some adult COVID-19 patients are also experiencing inflammatory responses, Mathew notes. Many of the most serious lung complications reported among COVID-19 patients tie back to inflammation in the body.
Like COVID-19, much is unknown about Kawasaki disease. Doctors aren’t totally sure what causes it, Jones says, but many believe it’s triggered by a viral illness. If there is a relationship between SARS-CoV-2 and Kawasaki, “I wouldn’t say that it would be that shocking to us,” Jones says.
When was Kawasaki Disease linked to COVID-19?

The first known published case of classic Kawasaki disease associated with COVID-19 was reported in Hospital Pediatrics in late April. A 6-month-old seen in Stanford, California, screened positive for COVID-19 after presenting with fever, blotchy rash, and minimal respiratory symptoms. She had initially been sent home from urgent care.
This week, the New York City Health Department announced finding 15 cases between April 29 and May 3. The “full spectrum of disease is not yet known,” it noted. “Only severe cases may have been recognized at this time.“
On Wednesday, the New York State Department of Health expanded that to 64 cases statewide and issued an advisory on what is being called “Pediatric Multi-System Inflammatory Syndrome Temporally Associated with COVID-19.“
In fact, as this article is being written, two children have died in New York with the syndrome, a 5-year-old boy, and a 7-year-old boy.
Italy, Spain, and the U.K. have noted an uptick in Kawasaki-like disease among children coincident with the COVID-19 outbreaks there.
British health authorities warned about a small rise in children with severe COVID-19 and features consistent with toxic shock syndrome and atypical Kawasaki disease. “Abdominal pain and gastrointestinal symptoms have been a common feature as has cardiac inflammation.“
Unusual Features
Even under normal circumstances, it can be difficult to sort out Kawasaki disease from other childhood diseases that cause similar symptoms given that there are no definitive blood tests, noted Michael Portman, MD, of Seattle Children’s Hospital and a member of the American College of Cardiology committee that set benchmarks for care of Kawasaki disease.
“What’s really unusual about this particular presentation is that they are older,” noted Deepika Thacker, MD, medical director for the cardiac inpatient unit at Nemours Children’s Health System in Wilmington, Delaware. Kawasaki disease typically affects children age 5 years and younger, but many of these cases reported have been in teens, she pointed out.
Other atypical features are the high prevalence of abdominal and GI symptoms.
In the NYC health department report, the 15 cases in children ages 2 to 15 years were hospitalized with typical or incomplete Kawasaki disease, some with shock. All had fever and more than half had rash, abdominal pain, vomiting, or diarrhea. However, less than half have had respiratory symptoms.
Some cases have even been described where severe abdominal pain sent these children to surgery but nothing was found, Thacker noted in an interview monitored by her institution’s media relations. Bloodwork has also been following a “very different pattern,” she said, including markers of cardiac injury higher than typically seen with Kawasaki disease.
“Whilst it is too early to say with confidence, features appear to include high CRP [C-reactive protein], high ESR [erythrocyte sedimentation rate], and high ferritin,” Britain’s Pediatric Intensive Care Society said in a statement.
The New York state alert also pointed to myocarditis and other cardiovascular changes that may be seen. “Additionally, some patients have developed cardiogenic or vasogenic shock and required intensive care. This inflammatory syndrome may occur days to weeks after acute COVID-19 illness.“
A press release from the American Heart Association (AHA) aimed to reassure parents of how uncommon the condition is but noted that as “some children are becoming very ill extremely quickly, children with these symptoms should be swiftly evaluated and cared for in hospitals with pediatric cardiac intensive care units, as needed.“
“Because there is a small but increasing number of children with fever and evidence of inflammation who are not severely ill, all children with unexplained fever and elevated C-reactive protein (CRP) or white blood cell count should be carefully monitored,” it urged.
The New York state alert agreed, calling on physicians not to delay seeking inpatient specialist input while trying to exclude other microbial causes.
The AHA’s Young Hearts Council said it is adopting the Royal College of Pediatrics and Child Health’s case definition, which doesn’t require a positive PCR test for SARS-CoV-2.
In guidelines for frontline providers that Thacker’s group is developing, a COVID-19 PCR test is recommended to be repeated after a few days, since it can come back negative initially. Antibody tests, too, are not very reliable, she said.
Aside from sensitivity issues with the tests, “it’s possible this is a late reaction to the virus,” Portman noted. In that intermediate period, active virus might not be found but antibodies being tested for might not have been generated sufficiently yet either.
Repeat echocardiography of the coronary arteries is needed too, because inflammation and aneurysm can develop during hospitalization for young people who come in with Kawasaki shock syndrome much like what has been described in the cases of “pediatric multi-system inflammatory syndrome temporally associated with COVID-19,” Portman noted.
Recommended inpatient treatment is to support shock (at least 75% need pressors), and give steroids and IV immunoglobulins, Thacker noted.
Missed Cases

While most children who develop Kawasaki disease recover without incident, “there’s still that 25% out there that if they get late treatment, they could have serious illnesses. And some of those children, the fever goes away and they’re walking around with a coronary artery aneurysm and they don’t even know it,” Portman noted.
“One of the fears with the COVID pandemic is that everyone has been told to stay away from hospital because they’re worried people will come to the hospital and be exposed,” he said. “But in fact, there are children we believe are out there, they have fever for 4 or 5 days, they call a line and are told, ‘well if it’s fever and nothing else your child’s not really sick, you don’t have to come and be evaluated.’ Some of those children could, in fact, have Kawasaki disease and be at risk for coronary artery disease.“
His group has seen fewer cases at its Kawasaki Disease Clinic during the pandemic than normally expected over the same period.
“This one child when we looked back at what happened a month ago, it looked like the child did have Kawasaki disease, eventually they were seen because of low-lying inflammation and fever,” he noted. While that child didn’t develop aneurysm, colleagues in other parts of the country have described children who did not come in or got delayed treatment and did develop aneurysm, he said.
The number of missed cases that lead to lasting harm is likely to be small, Thacker noted.
Still, Portman urged general practice physicians, pediatricians, family physicians, and emergency physicians to continue surveillance for Kawasaki disease and not assume a child is fine because they don’t have respiratory symptoms.
Open Questions
Kawasaki disease has long been believed to be an immune response triggered by infection, but its etiology is still not clear and not all viruses predispose to Kawasaki disease, Thacker noted.
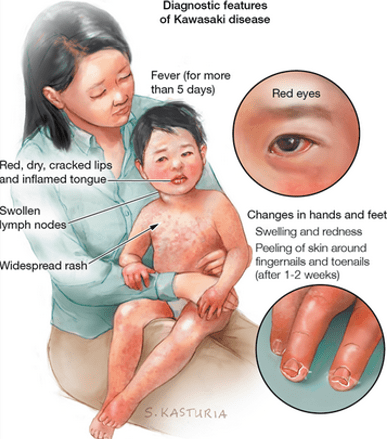
And despite the chronological connection between COVID-19 and these cases, “at present, there is no definitive evidence that COVID-19-induced shock is related to Kawasaki disease,” cautioned Anne Rowley, MD, an infectious diseases specialist studying Kawasaki disease at Northwestern University in Chicago.
“Some clinical symptoms of both these disorders — Kawasaki disease and COVID-19 — such as fever, rash and eye redness (conjunctival injection) are present in many childhood illnesses. However, the laboratory testing of these two groups of children seems quite different, and in particular, the children with COVID-19 infection have inflammation of the heart muscle rather than the characteristic swelling of the coronary arteries that are observed with Kawasaki disease.“
To better understand what’s going on, the AHA council called for enrolling affected children in COVID-19 studies that obtain serum or plasma samples.
Portman’s group is looking to track Kawasaki disease patients to see if they were exposed to COVID-19, to look for genetic susceptibility, and to see what happens to their immunity to the coronavirus.
It’s possible that IV immunoglobulin treatment could prevent the patient from developing full immunity to the virus, Portman noted, pointing to recommendations from the American Academy of Pediatrics calling for live immunizations for 11 months after use.
On a broader scale, one community-based study is the National Institute of Allergy and Infectious Diseases (NIAID)’s 6,000-person HEROS study looking into the rate of SARS-CoV-2 infection in U.S. children and their family members, which collects nasal swab and blood samples from participants every 2 weeks.
“One interesting feature of this novel coronavirus pandemic is that very few children have become sick with COVID-19 compared to adults,” said NIAID Director Anthony Fauci, MD, in a statement. “Is this because children are resistant to infection with SARS-CoV-2, or because they are infected but do not develop symptoms? The HEROS study will help us begin to answer these and other key questions.“
If all the attention on Kawasaki disease with COVID-19 drives data collection, the enigmatic disease could end up being better understood and treated as well, Thacker suggested.
Worth Watching

Diagnosis of classic Kawasaki is made on the basis of fever lasting more than 5 days, plus four out of five diagnostic criteria like the ones above disclosed.
While most children are asymptomatic or exhibit mild symptoms from COVID-19 infection, the symptoms of Kawasaki disease are very visible and should be taken seriously.
Kawasaki vasculitis, which is one of the consequences of untreated cases, is the leading cause of acquired cardiovascular disease in children, and it can lead to death.



