BA.5 Shows COVID Is Evolving Fast. Why Aren’t We Fighting Back?

We’re still in the midst of one of the largest COVID waves of the pandemic, and it’s fueled by the Omicron BA.5 subvariant, the most contagious and most immune-evasive coronavirus strain yet. Scripps’s Dr. Eric Topol, who has been one of the loudest voices sounding the alarm over BA.5, has repeatedly described the strain as the “worst” COVID variant on account of it having more fitness, growth advantage, and immune evasion than any of its predecessors. According to the latest CDC estimate, BA.5 now accounts for nearly 82 percent of all new infections in the U.S., where it has prompted a surge in reported cases, test-positivity rates, COVID wastewater levels, and, thanks to its immune evasion, reinfections. Last week, it even infected President Biden with his first-ever COVID case; this week, an outbreak hit the Senate.
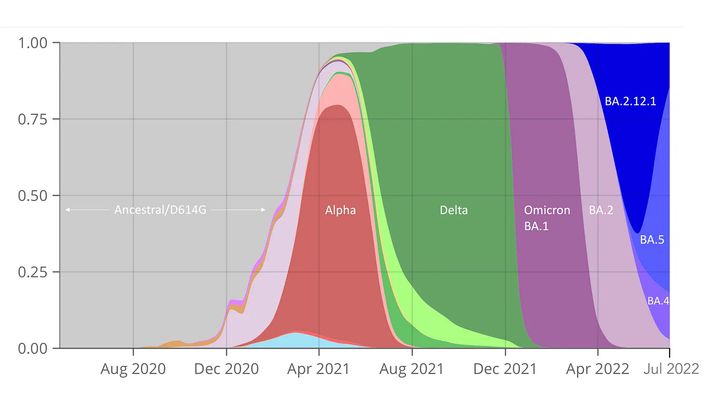
The BA.5 wave has also been driving up the number of U.S. hospitalizations, along with a slight rise in the number of COVID deaths, but it hasn’t produced severe outcomes anywhere near the scale seen in previous major waves. Indeed, the rapid onset of BA.5 and its subvariant brethren (BA.4, BA.2, and BA.2.12.1) without a corresponding surge in severe COVID has prompted a sense that we’re finally in a new phase of the pandemic where new strains come and go, COVID continues to spread and surge and unsettle, but our bolstered immune systems hold the line and we avoid the recurring nightmare of mass illness and death.
Scientists are still studying the new variant, and the BA.5 wave has been playing out differently in various countries, likely due to a complicated combination of factors. But while the far less severe impact of the BA.5 wave in the U.S. has, thus far, been a welcome departure from what we’ve encountered before, some COVID experts, like Topol, remain concerned. Though it’s been more than two and a half years since COVID arrived, we’re still not staying ahead of the virus.
Topol and immunologist Akiko Iwasaki just co-wrote a paper calling for an accelerated Operation Warp Speed–like initiative to pursue nasal COVID vaccines, which could provide mucosal immunity that stops the virus in the part of the body where it starts. Topol has also pushed for the development of other potentially variantproof vaccines, like pan-sarbecovirus and pan-coronavirus vaccines. This week, the White House hosted a summit on future COVID vaccines attended by many of the top minds in the field, including Iwasaki, but it’s far from clear that any of the promising ideas and goals discussed there will get the government funding they’d need to have an impact on the pandemic anytime soon.
I recently had a long conversation with Topol about BA.5, why he’s troubled by it, and what the variant and its arrival portend for the future.
On one hand, here in the U.S. we’ve seen a significant drop in hospitalizations and deaths amid the wave of cases of BA.5 and the other earlier Omicron subvariants. But you’ve been calling attention to the fact that in some other countries, BA.5 has fueled some alarming spikes in cases, hospitalizations, and even deaths. So, is the U.S. through the worst of this?
I agree that, overall, if you look at it globally, hospitalizations and deaths from BA.5 are not going to reach levels anywhere close to Omicron or previous waves, but they’re not trivial elevations. Deaths are going up over the whole world from BA.5. Our wave is still playing out right now. We’re poorly vaccinated here in the U.S. — poorly boosted, especially in high-risk people like seniors. So I wouldn’t want to conclude that we’re out of the woods. We could be in for more trouble before the BA.5 wave is finished.
I’m actually a very optimistic person. When we were coming down from Delta and had not seen Omicron, I thought, Wow, the worst is over. Then Omicron proved to be an onslaught in terms of spread by any metric as well as the toll it took in more serious outcomes. So with that background, the recent CDC report that came out about the vaccines really has me worried.
Why’s that?
It’s not like all of a sudden there’s going to be a variant with total immune escape from vaccines. But in the CDC morbidity and mortality report, it said that two-dose vaccine effectiveness against hospitalization for the original BA.1 Omicron strain — we’re not talking about infections because we’re well past having good vaccine coverage for that — but for hospitalization, it dropped to 61 percent for two doses. And for BA.2 and BA.2.12.1, the latter of which is more like BA.5 but not as bad, two doses against hospitalization dropped to 24 percent. That should set off alarms because we don’t have a lot of people with a third shot. For three shots the efficacy jumped back up, but only to 52 to 69 percent with BA.2/2.12.1.
Kaiser Southern California has also had two reports on vaccine effectiveness in their big network of patients, and they show the same attrition against hospitalizations as was seen in this much larger new comparison from the CDC.
So how can you feel good about these data? I don’t see how. This narrowing benefit of the vaccines, which I think is due to more immune escape, not due to more infections in the unvaccinated, it’s still a very big gap. To drop down almost 40 points in effectiveness against hospitalizations with only two shots — this should be a signal that something is going on with our vaccine protection. But you don’t see anybody raising concerns about this. All you hear is happy talk that we have great protection from hospitalizations and deaths. I don’t know about that. These data don’t support that.
So that suggests that hospitalizations will likely keep going up in the BA.5 wave?
Yeah, they’re going to go up. The number of current U.S. hospitalizations is already over 40,000. I wouldn’t be surprised if it gets to 50,000 or 60,000. It isn’t going to get near 160,000, like it did with BA.1, only because so many people got infected with BA.1 and there’s some cross-immunity. But the number of hospitalizations has been going up substantially. It had gotten down to 12,000 and now back up past 40,000. If you look at the curve, it has a new increased slope since BA.5 started to take effect, and it’s still on the way up. The question is does it get to 50,000? Does it get to 60,000? That’s a lot of sick people in the hospital.
And the other thing I would just say, parenthetically, is with BA.5, I’ve never seen so many infections in my personal network, including family, friends, colleagues. I’ve never seen infections last as long. After 10 days, still testing positive, after day 12, 13, 14. The behavior of BA.5 is different — and the fact that our CDC still adheres to this five-day isolation recommendation, it’s incredulous. They’re actually promoting spread by doing that.
There’s no question that this is a different effect from BA.5 in terms of the length of infectiousness, how much it’s spread, and maybe not more hospitalizations. But remember, that’s with Paxlovid, which now has 90 percent efficacy in preventing hospitalizations for high-risk people.
Right, if a variant emerges that Paxlovid isn’t as effective against, that could suddenly leave us much more vulnerable to severe COVID again.
Yes. And I think most of us who’ve really zoomed into the mutations on MPro, the main protease of the virus that Paxlovid works on … I’d say it’s just a matter of time. It’s inevitable. Already these mutations have appeared naturally because of the pressure that the virus is getting from Paxlovid. It’s inevitable. We’re going to see resistance to this drug, which, after the vaccines, is the second-most-important advance that we have had to take on the virus. But it may be short-lived, it could be that by year’s end or the beginning of next year, we won’t have Paxlovid as a remedy or rescue anymore. There’s no question Paxlovid is helping keep the hospitalization number down.
Updated booster shots that better target the Omicron lineage are on the way. Will those help us stay ahead of the virus?
We need variantproof boosters. No more chasing variants because we are not very good at that. Just get the vaccines that would take on all sarbecovirus and betacoronavirus so we can put an end to the whole idea of trying to anticipate the variant that we’ll need a booster for. We know how to do that. We have over 25 incredibly potent broad neutralizing antibodies. We can make vaccines that induce several of those antibodies to never have to worry about a variant in terms of having protection.
But those aren’t the boosters arriving this fall.
No. The booster plan is for BA.5. And saying that will be here for the fall is highly optimistic. It took seven months to get a BA.1 booster. Then the government sent the pharmaceutical companies back to go get us a BA.5 booster. Thinking that could be available in October or November — that’s highly optimistic. And we certainly don’t know what variant is going to be with us at that time. It won’t be BA.5 anymore. There’ll be something else that will outcompete BA.5. Once that BA.5 booster is available, it may not work against the then circulating virus because it knows how to evolve.
Why aren’t these better boosters in the pipeline instead?
Well, it’s pretty clear that Congress is unwilling to fund a dollar more for COVID. And that’s, of course, the Republicans blocking any COVID bill. But there are even people in the Biden administration who aren’t sure how much these next-generation vaccines — including variantproof, universal, and nasal — are going to help us. That’s just, I think, being out of touch with the science. And any COVID bill dedicated to getting ahead of the virus would need to include better drugs, more drugs. Because we have to plan for Paxlovid’s obsolescence, and we don’t have anything to replace it yet — but there are many good candidates in the pipeline.
There seems to be at least anecdotal evidence that a small number of people are now getting reinfected within a matter of weeks. What do you make of that?
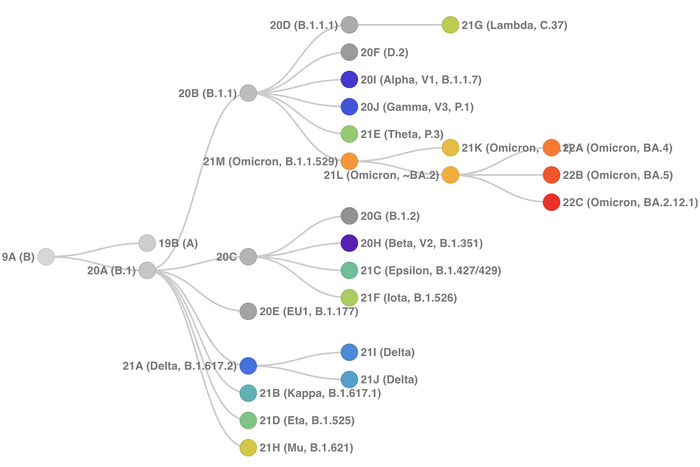
Those added mutations that we first saw with BA.2.12.1 and now in BA.4 and BA.5 — that immune evasion is what’s responsible for all these early reinfections. That’s where this virus is going. It’s got a flashing light: “I have found ways to evade your immune system, and I can keep building on that.” Reinfection is perhaps the best real-time signature of immune evasion.
What’s your sense of where long COVID is going? Is there any other way to avoid it than just not catching regular COVID in the first place, which is clearly getting harder to do at this point in the pandemic? Is there some other way to handle it?
Well, you’re right. Avoid the infection, first. Then, if you had a vaccine, that seems to avoid the chance of long COVID to some extent, but we also have to have treatments for it — we don’t have any yet that are validated. We have a billion dollars from the NIH toward long COVID, but you’re not seeing any real contributions that funding has advanced yet. And we know that long COVID is not a homogeneous disorder. There are different components. Some are much more immune-mediated, some are much more autonomic nervous system-mediated. So there’s a lot to unpack with that.
So what are you most worried about with regard to the future evolution of SARS-CoV-2?
The known unknown, which is that this virus still has many more ways to become more resistant to our immune response — and we should plan on that. We keep thinking we’ve reached some kind of limit. But the most important lesson from BA.5, to me, is that it’s worse. If it had come without BA.1 as a predecessor … the only reason BA.5 doesn’t look horrific right now is because BA.1 had built up the immunity wall. More than half of Americans have had BA.1 or BA.2. And we’re now seeing in BA.5 the most innovation, the most growth advantage, the most fitness of the virus yet — and we’re just not dealing with it.
If some people think, Oh, it can’t get worse, it’s going to get better. We don’t know that. You have to plan for the worst-case scenario. And the worst-case scenario is that the virus further increases its immune evasion. It’s already picking up things that worked in prior versions of the virus: For instance, BA.2.12.1 and BA.5 have the same key L452R mutation that the Delta variant had. Anyone who thinks the virus doesn’t have room to evolve further is just not paying attention.
Is that a near-term threat? Can we predict a timetable for any of this evolution?
No, but it’s accelerating. We know that much. The time it’s taken to get from BA.1 to BA.5 is not a good tempo for a whole new lineage to outcompete the prior one and achieve dominance worldwide.
So it doesn’t look good. These new strains are clearly happening more frequently than they used to. In the first 12 months of the pandemic, there was no evolution of the virus. We basically had the original Wuhan strain, and then D614G, which arguably only had minor functional consequences. Alpha was mild compared to anything we’ve seen subsequently, then there was Delta, which obviously had more infectiousness and virulence. But now, with this whole Omicron family, it’s moving at a very rapid pace.
We can’t predict the new mutations. We can’t predict the timing. We can try to extrapolate, but even extrapolating, we had no good semblance of what Omicron would look like with its 57 spike mutations in BA.1. No one accurately predicted we would be looking at that.
And it’s too fast.
It’s the known unknown. Yeah.
UCL Genetics Institute director Francois Balloux recently explained that he wasn’t as concerned about the emergence of further Omicron subvariants as he was about the reemergence of COVID lineages, like Delta, that have undergone a kind of underground evolution. So a strain circulating in some isolated part of the world; or one within an “animal reservoir,” i.e. an animal population the virus has spilled into from humans; or one that has evolved via a long-term chronic infection in someone who is immunocompromised — which is how many scientists believe Omicron itself evolved. How worried are you about these paths?
When an immunocompromised person gets infected, they really can’t mount a good immune response. So the virus, instead of what it’s been doing globally for two and a half years, goes through this accelerated evolution in that person, picking up mutations left and right. It basically has unchecked potential to evolve in that person, and then that evolved virus infects other people. That’s pretty certainly what happened with Omicron.
I agree that the animal reservoirs are also a concern because we’ve already seen spillover to many different species, including hamsters, mink, cats, and deer. So that’s another way that the virus can evolve, in an animal reservoir, and come back to spillover in humans.
We also haven’t contained the virus around the world, so it can continue to evolve through the millions of infections each day. And there are tens of millions of immunocompromised people in the world. It just takes one person, really, to trigger things. And then you have all these hybrid versions of the virus that we’re seeing, all these recombinants, which could bring about the worst elements of different parts of the virus. Most of the public focus on the evolution of SARS-CoV-2 has been spike-centric, but there are lots of other parts of the virus that can be troubling, that can make the virus more difficult to deal with. So again, there’s lots of room for this virus to go.
There are too many paths. If you’re just taking odds, and you have all these different routes and tens of millions of people that are immunocompromised around the world, are you going to bet against the virus evolving into something that’s more challenging than what we have today? I don’t think so.
Is there anything we can do to defend against COVID strains spilling back over from animal populations?
No. No defense at all, unfortunately.
You and some other scientists have suggested that Omicron and particularly BA.5 are so different from any previously dominant COVID strains that in many ways we are now effectively dealing with a new virus. You’ve also pointed out that if the original Omicron strain had the characteristics of BA.5, the Omicron wave would have been far worse. I understand that’s a way to highlight why people should be concerned about BA.5 and what it means for COVID’s evolution, but is that actually possible? Can a BA.5 evolve on its own without there first having been a BA.1?
It’s a good question because we don’t really know how BA.5 evolved. We just know it did. And could BA.5 have come in from an immunosuppressed person de novo without BA.1? Possibly. We just don’t know. Basically new mutations showed up. Four key mutations showed up beyond BA.2 that have caused a lot of trouble, but we don’t really know precisely how that occurred.
But we know why it occurred.
Yeah. The virus is under pressure from vaccines and prior infections and now Paxlovid. So it’s finding ways to stand up to find new hosts. All viruses want is to find a new host. So they just keep mutating, and some of them don’t work. Most of them fortunately don’t work, but a lot of them do, and those are what we’re seeing.
Meanwhile, globally, we’re still giving COVID as many opportunities to evolve as we were a year ago — if not more because now there are reinfections.
Yeah, if not more. We’re putting pressure on the virus to find new ways to circumvent our immune response — and that’s what it continues to do.
And at the same time, we’ve collectively done virtually nothing to prepare for whatever evolves next.
Right. From day one of this pandemic, we have never tried to get ahead of the virus. Labs have come up with all sorts of broad neutralizing antibodies that would be variantproof. Nasal vaccines, to block transmission, to achieve mucosal immunity — there are 12 in clinical trials. There are all these drugs in the hopper. Pan-coronavirus vaccines. These are all academic pursuits or largely from small companies. There hasn’t been a national or a much larger international initiative to get ahead of the virus.
By initiative, you mean money.
Money and an Operation Warp Speed 2, with collaborations and private-public industry partnerships. And not necessarily just the U.S., it should be global. But you don’t see that, and it’s so stupid because look how successful we were. Operation Warp Speed showed how good we could be at this. But we haven’t done anything. We keep reacting and chasing instead of doing the things we know would get ahead of it.
I look at the data, and it says we can do better than this. I know we can; the science is there. It’s just waiting in the hopper to be activated, but we’re just not taking it seriously enough. And I want to get out of this thing. I thought we were out of it as we came down with Delta in June 2021. Who would’ve thought we would get to now, a year-plus later, and there’s still no light ahead of us? That’s why I want to take the aggressive get-ahead stance.
It seems like political will for that stance is nonexistent in the U.S. right now.
It’s also internationally. You don’t see the U.K. — which has been a model for science in the pandemic — or many places around the world that are capable of it talking about going after pan-coronavirus vaccines. Why aren’t we making this a global priority?
I’m optimistic that we can seize and achieve containment of the virus once and for all. I’ve been optimistic like that for many months, but I feel like I’m a Lone Ranger — not a single voice, but one of a minority.
To be clear, you mean a pharmacological way to contain the virus. Because we’re never going back to nonpharmaceutical interventions like we saw in the first few years of the pandemic, or at least unless there’s an enormous rise in hospitalizations and deaths.
Yeah. In January 2021, my colleague Dennis Burton and I wrote in Nature that we need a variantproof vaccine. This virus is ideally suited, as compared to flu or HIV, for a variantproof vaccine. The initial success of Pfizer’s vaccine was 95 percent against symptomatic COVID. There’s never been a flu vaccine like that. Look at the success of Paxlovid: a 90 percent reduction in hospitalizations and deaths. This virus is vulnerable. We’ve proven that. We’re just not building on our successes. It’s incredible. This is a less challenging, less hypermutating virus than the flu. Our COVID vaccines make flu vaccines look like a joke, or at least they did.
So we already have COVID on the ropes and can finish it off — if we try.
That’s why I’m so optimistic. We can do this. But we’re not doing it.
This interview has been edited for length and clarity.